Degenerative Disc Disease
Progressive wear of the intervertebral discs that can lead to chronic back or neck pain, stiffness, and reduced functional capacity over time.
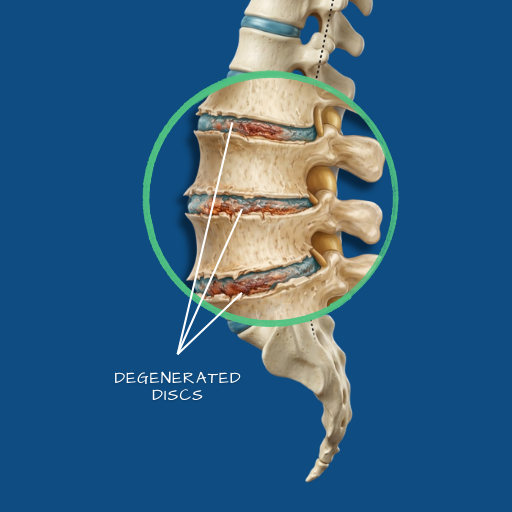
Overview
Degenerative disc disease is not a disease in the traditional sense — it is a term used to describe the natural age-related breakdown of the intervertebral discs that cushion the vertebrae of the spine. These discs lose water content, height, and resilience over time, reducing their ability to absorb load and distribute movement evenly across spinal segments. In most people, some degree of disc degeneration is present by middle age and causes no symptoms at all. In others, the degenerative process leads to chronic pain, stiffness, and progressive limitation of daily activity. The condition most commonly affects the lumbar spine (lower back) and cervical spine (neck), and it can develop alongside or contribute to other spinal conditions including disc herniation, spinal stenosis, and spondylolisthesis.
Causes
The primary cause is age. As the discs age, the water-rich nucleus pulposus at the centre dries out and the outer annulus fibrosus becomes less flexible and more prone to small tears. This process is accelerated by certain factors — prolonged physical loading such as heavy manual work or repetitive lifting, a sedentary lifestyle that weakens the supporting musculature, smoking (which reduces vascular supply to the discs), obesity, and a genetic predisposition to early disc ageing. Prior spinal injury can also initiate or accelerate degenerative change at a specific level. In working professionals, the combination of sustained sitting posture and reduced physical conditioning is a common contributing pattern.
Symptoms
Symptoms vary considerably between patients. The most common presentation is a dull, persistent ache in the lower back or neck that worsens after prolonged sitting, standing, or physical activity, and temporarily improves with movement or position change. Stiffness after rest — particularly on waking — is common. Some patients describe intermittent episodes of more acute pain on top of a chronic background ache. Where degeneration has reduced disc height significantly, nerve root irritation may produce radiating pain, numbness, or tingling into the arms or legs. A notable feature of degenerative disc disease is that the degree of degeneration seen on imaging does not reliably predict the severity of symptoms — patients with extensive degeneration on MRI may have minimal pain, while others with modest changes may be significantly affected.
Diagnosis
MRI is the investigation of choice, providing detailed information on disc hydration, height loss, annular tears, and any secondary changes to the vertebral end plates. X-rays are useful for assessing disc height loss and vertebral alignment. Standing X-rays in particular reflect the functional load on the spine in a way that lying-down MRI does not. Clinical examination — assessing range of movement, neurological status, and the specific movements or positions that provoke symptoms — is essential for correlating the imaging with the patient’s actual experience.
Conservative Care
The majority of patients with degenerative disc disease are managed effectively without surgery. Physiotherapy focused on core stabilisation — strengthening the deep spinal and abdominal muscles that support the degenerating segments — is the foundation of conservative management. Aerobic conditioning, postural correction, and ergonomic review for desk-based workers are equally important. Pain management, including anti-inflammatory medications and selective nerve root or facet joint injections, can provide periods of relief that enable meaningful engagement with physiotherapy. Conservative management is the appropriate long-term framework for most patients, with surgery reserved for those who meet specific clinical criteria.
Surgical Indications
Surgery for degenerative disc disease is considered when conservative care has been thoroughly and consistently applied without adequate relief, when the patient’s functional capacity is significantly and persistently impaired, or when degenerative changes have produced secondary conditions — stenosis, spondylolisthesis, or significant nerve compression — that themselves meet surgical criteria. Imaging findings alone, however extensive, are not a sufficient indication for surgery. The clinical picture — symptoms, functional impairment, and neurological status — drives the decision.
Surgical Approach
Where surgery is indicated for degenerative disc disease at a specific level, the procedure is typically a spinal fusion — stabilising the affected segment to eliminate the painful movement occurring at the degenerated disc. This is performed using a posterior or transforaminal lumbar interbody fusion (PLIF or TLIF) approach, in which the degenerated disc material is removed, a structural cage is placed in the disc space to restore height and alignment, and pedicle screws provide stabilisation. The Medtronic StealthStation navigation system is used for accurate pedicle screw placement, reducing positional error in a procedure where precision directly affects outcome. A minimally invasive approach is used where anatomy and the extent of degeneration permit.
Recovery
Recovery from fusion surgery for degenerative disc disease follows a staged progression over three to six months. Early recovery involves activity restriction, wound management, and the beginning of gentle mobilisation. Physiotherapy becomes progressively more active from four to six weeks post-operatively, focusing on building the strength and movement patterns needed to support the fused segment. Return to desk-based work is typically possible within six to eight weeks. Return to physical activity and manual work takes longer, guided by clinical progress and imaging confirmation of fusion consolidation. Patients are counselled that fusion addresses the painful segment but does not halt degeneration at adjacent levels — long-term spinal health requires ongoing conditioning and lifestyle attention.
If back or neck pain has become a persistent feature of your daily life, a structured evaluation is the starting point for understanding your options.