Vertebroplasty / Kyphoplasty
Minimally invasive procedures to stabilise painful vertebral compression fractures — most commonly from osteoporosis — by injecting bone cement into the fractured vertebra.
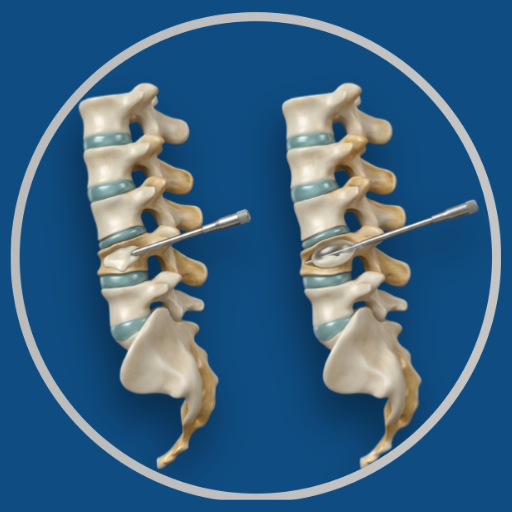
Overview
Vertebroplasty and kyphoplasty are percutaneous procedures performed through small skin punctures under imaging guidance. In vertebroplasty, bone cement (polymethylmethacrylate, PMMA) is injected directly into the fractured vertebra under pressure. In kyphoplasty, a balloon is first inflated inside the vertebra to restore some of the lost height before the cement is injected into the cavity created. Both procedures stabilise the fracture and significantly reduce pain in the majority of patients. Kyphoplasty offers the additional benefit of partial height restoration and a lower risk of cement extravasation.
Before Surgery
MRI to confirm the fracture is recent and active (bone oedema on MRI indicates the fracture is the pain source). CT to assess fracture morphology and plan the approach. Medical assessment including bone density evaluation. Patients on anticoagulants require specific management before the procedure.
During Surgery
Performed under local anaesthesia with sedation, or general anaesthesia for anxious patients. The patient is prone. Needles are placed into the fractured vertebra through the pedicles under fluoroscopic guidance, bilaterally. In kyphoplasty, balloons are inflated to restore height before cement injection. Cement is injected under controlled conditions with continuous fluoroscopic monitoring to detect any extravasation. Duration is typically 45–90 minutes.
After Surgery
Patients are typically mobile within a few hours of the procedure. Hospital stay of 1–2 days. Pain relief is often experienced rapidly — within 24–72 hours in most patients. Wound care involves small dressing changes only.
Recovery
Recovery is faster than from any open spinal procedure. Return to light activity within 1–2 weeks. The underlying bone health issue — osteoporosis — requires ongoing medical management to reduce the risk of further fractures at adjacent or other levels. This is addressed as part of the post-procedural care plan.
Dr. Viswanath's Approach
Patient selection is the most important factor in achieving good outcomes from cement augmentation procedures. The fracture must be confirmed as recent, active, and the primary pain source — and the patient’s overall bone health and medical status must be optimised. The procedure is performed under careful fluoroscopic guidance with attention to cement volume and containment.
Medical Disclaimer: This information is provided for educational purposes only and does not constitute medical advice.